Préparation préopératoire (Avant)
Left colectomy
Left colectomy
Operation
Indications for left colectomy – resection left colon – sigmoid resection – anterior resection:
– Left colon cancer – sigmoid cancer
– Left colon perforation – sigmoid perforation
– Left colon polyp – sigmoid polyp (if resection not possible via colonoscopy)
– Left colon ischemia – sigmoid ischemia
– Benign tumor of the left colon – sigmoid
– Volvulus of the sigmoid
Includes resection of part or all of the left colon up to the rectum under general anesthesia, with restoration of continuity between the transverse colon or the remaining left colon with the rectum.
In the first stage of surgery, the colon is mobilized without injuring the blood supply, by freeing the attachments of the colon from the abdominal wall and sometimes even the attachments to the spleen and stomach. Mobilization of the colon is necessary to achieve a tension-free suture/anastomosis in the final stage of the procedure.
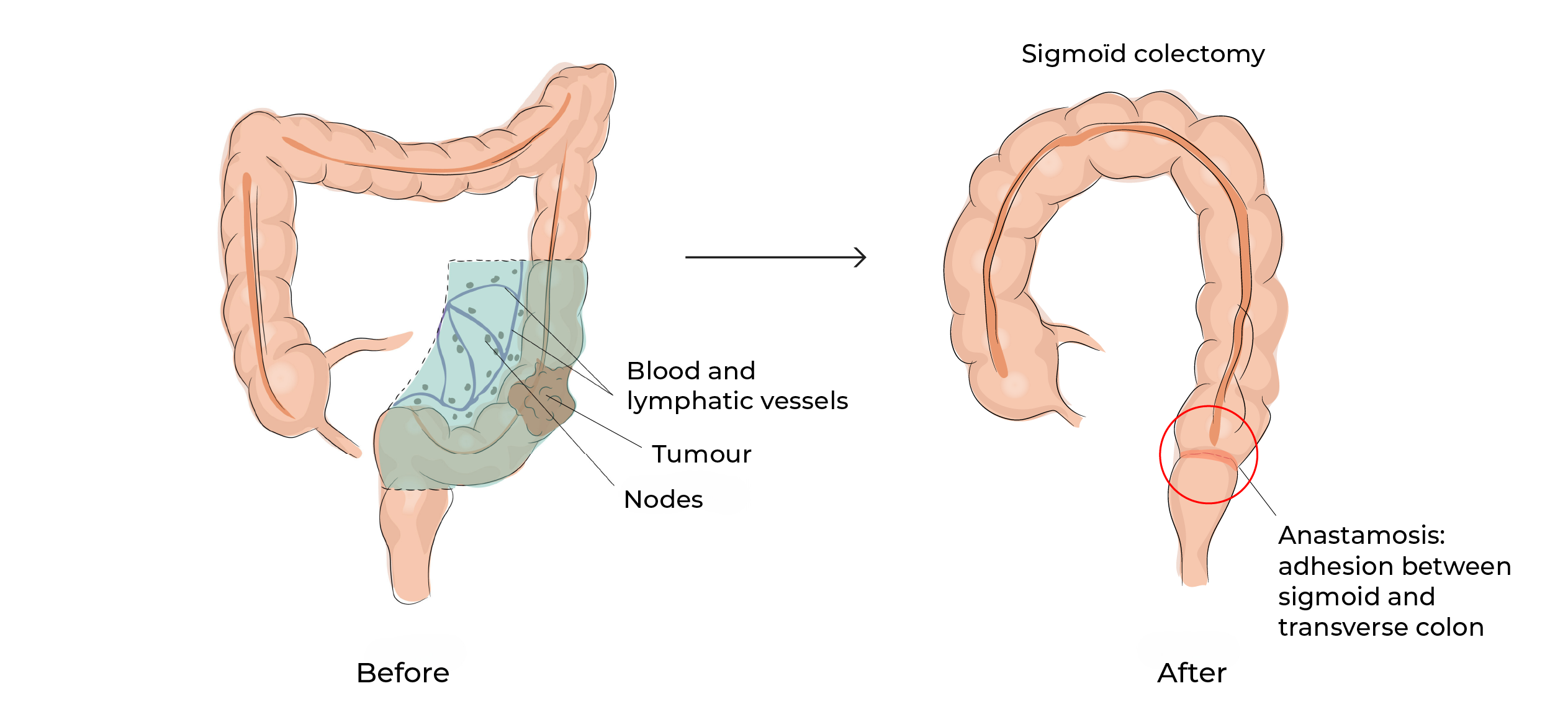
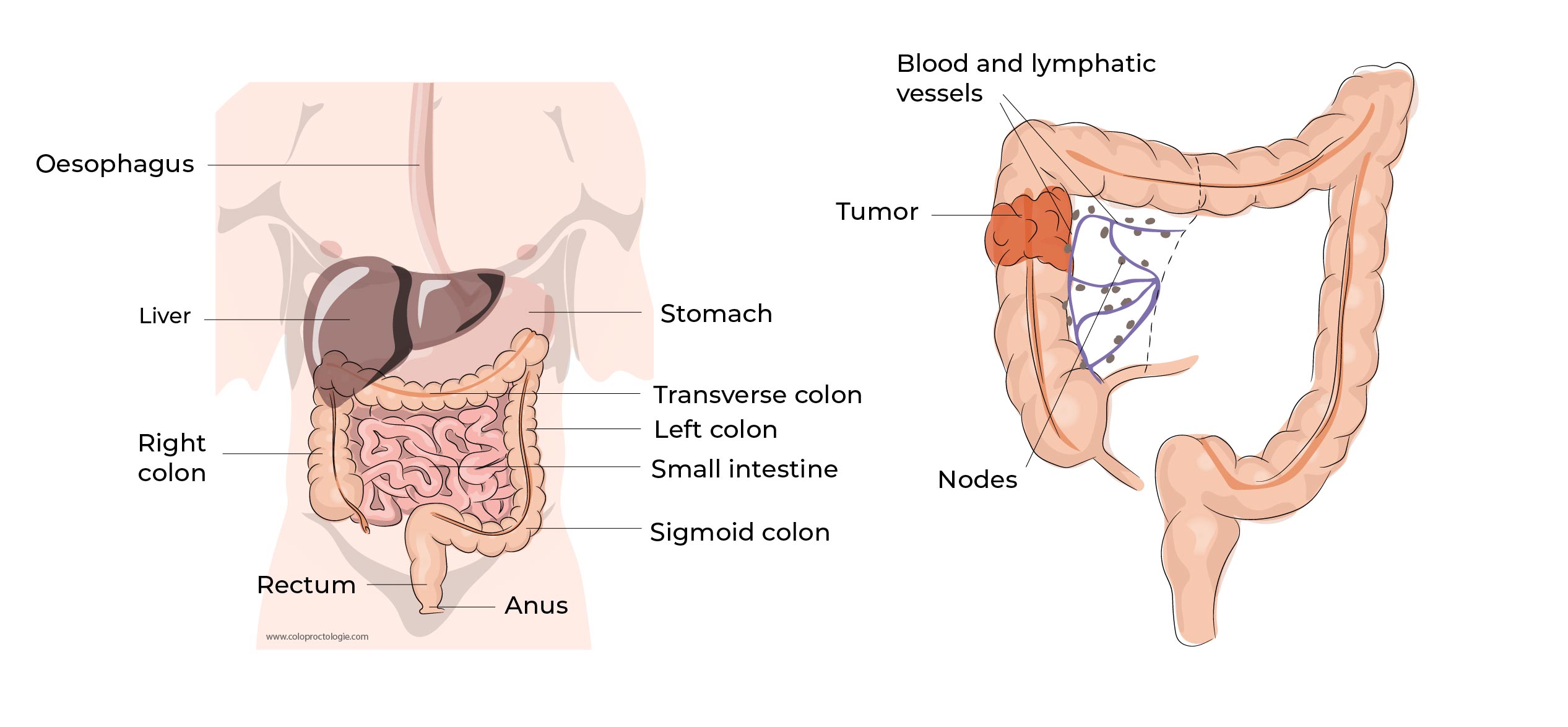
In the second stage of the procedure, the colon together with the surrounding fatty tissue containing the blood vessels and lymphatic tissue (lymph nodes) of the colon are removed , ” en block ” (in one piece). The tumor with its fatty envelope is removed from the abdominal cavity through an incision in the lower abdomen( pubic region) or in the left lower abdomen.
The removed lymphoid tissue is examined for the presence of tumor cells in the lymph nodes.
The presence of tumor cells in lymph nodes is an important factor when deciding whether or not to administer adjuvant chemotherapy.(chemotherapy after surgery).
In the third stage, continuity is restored with an anastomosis / suture made of staples (titanium) with a machine inserted through the anus.
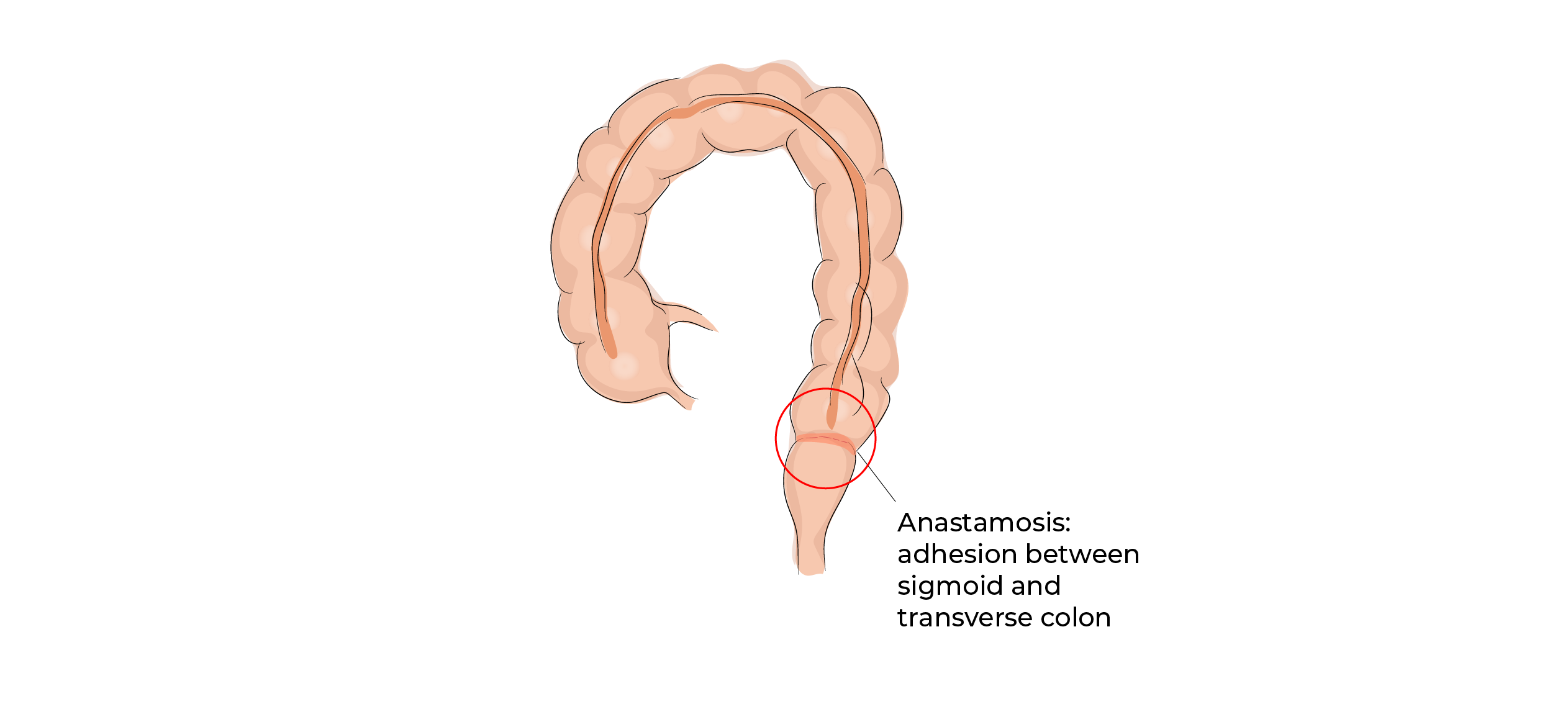
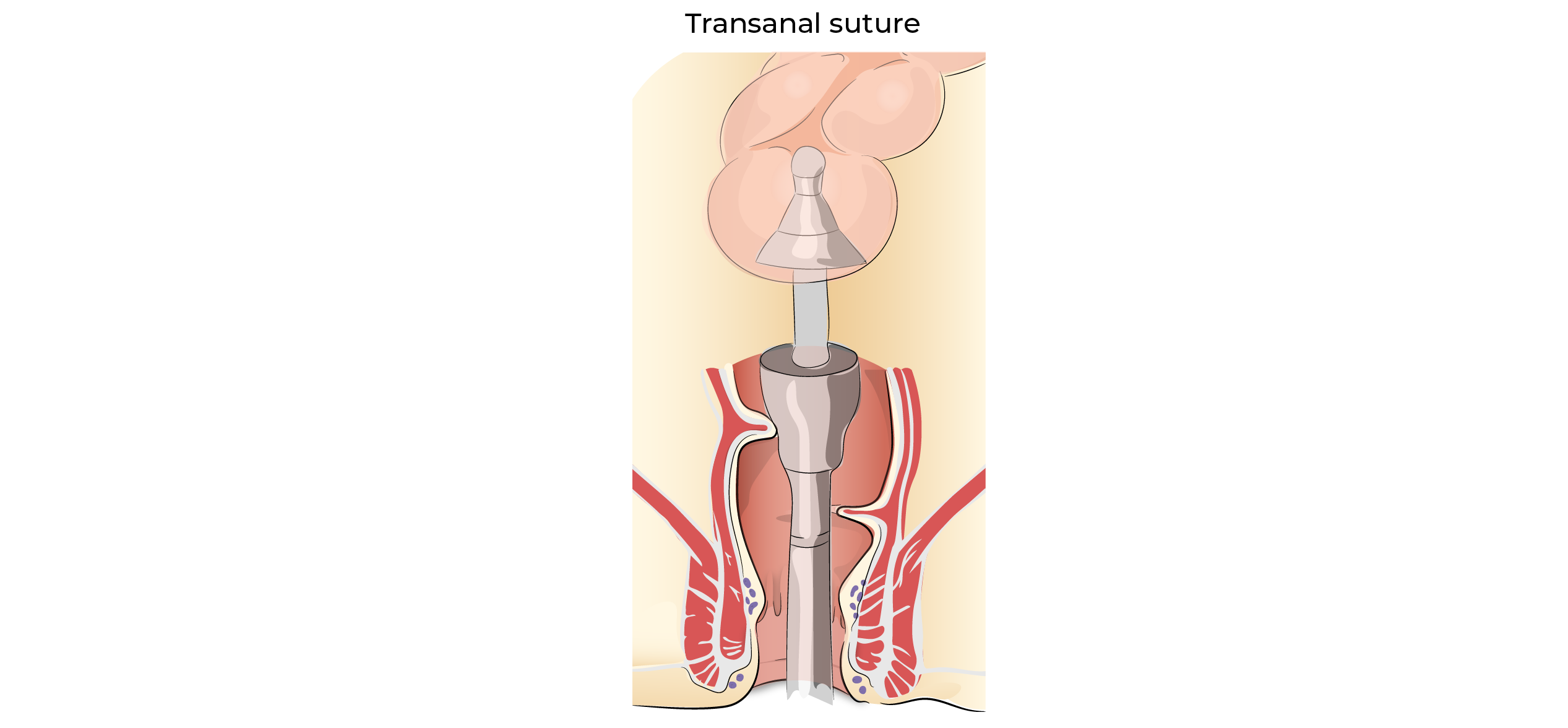
Advantages:
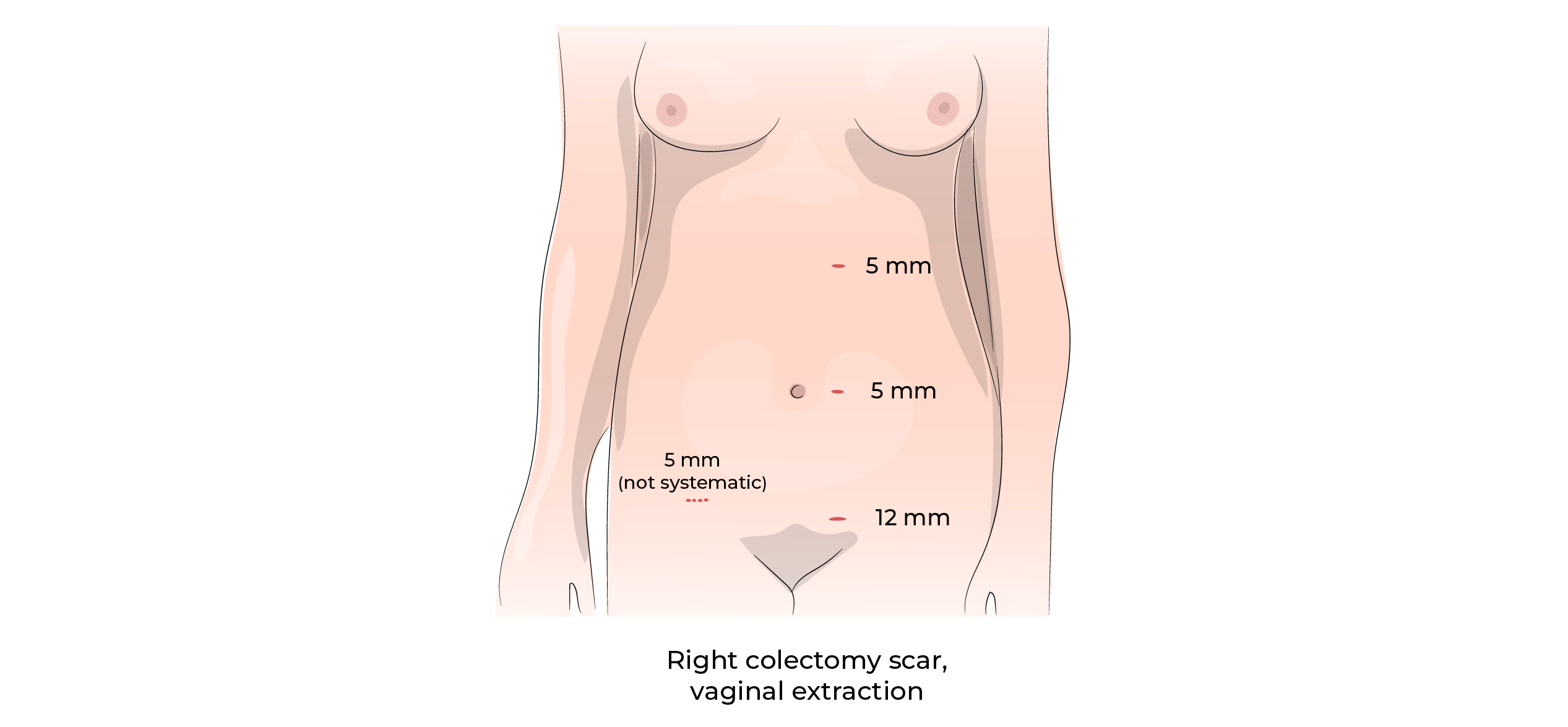
Laparoscopy may not be possible when:
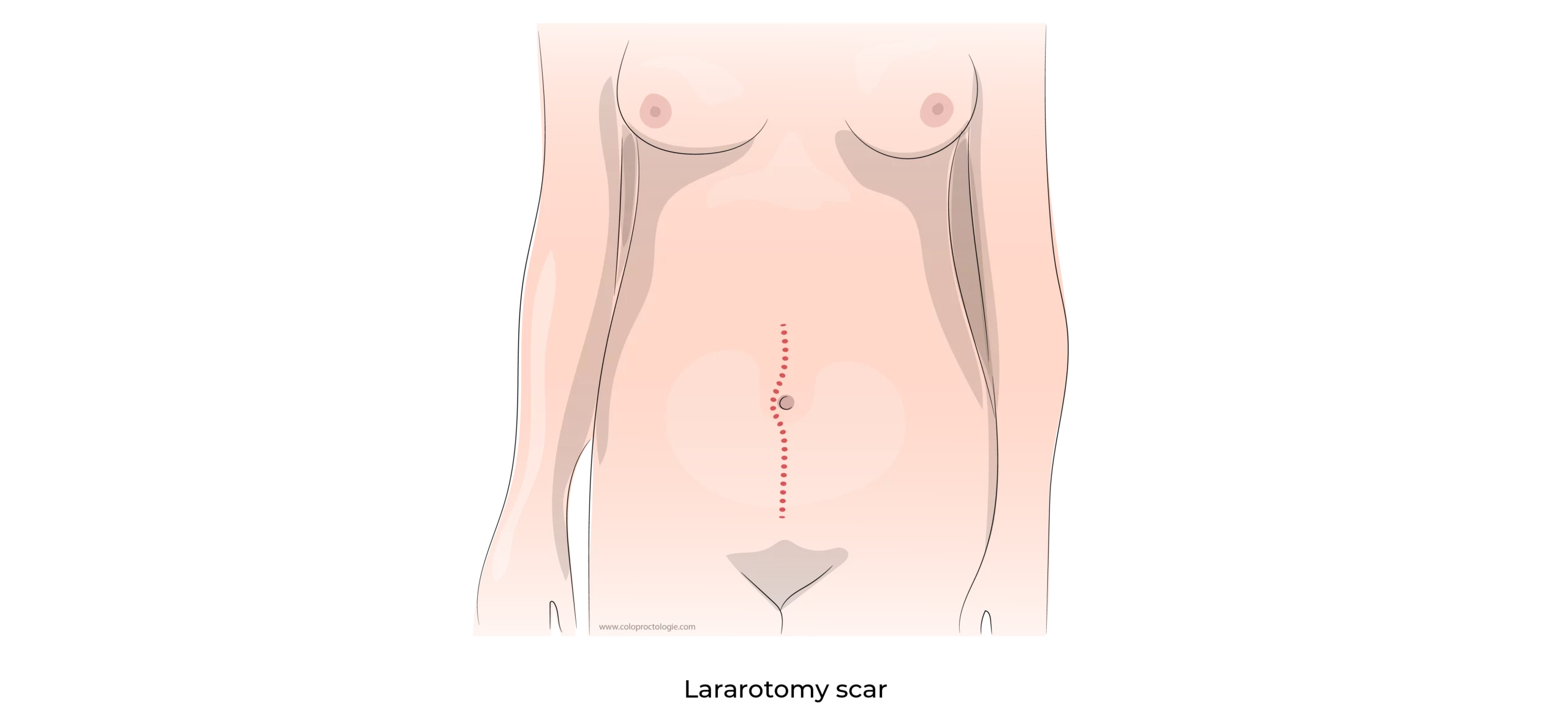
Factors that increase the risk of complications:
Incidence : 3 – 8 %
A stoma is a surgical procedure in which the bowel is sutured through the abdominal wall earth the skin so that the fecal matter is discharged via in a pouch / bag attached to the skin.
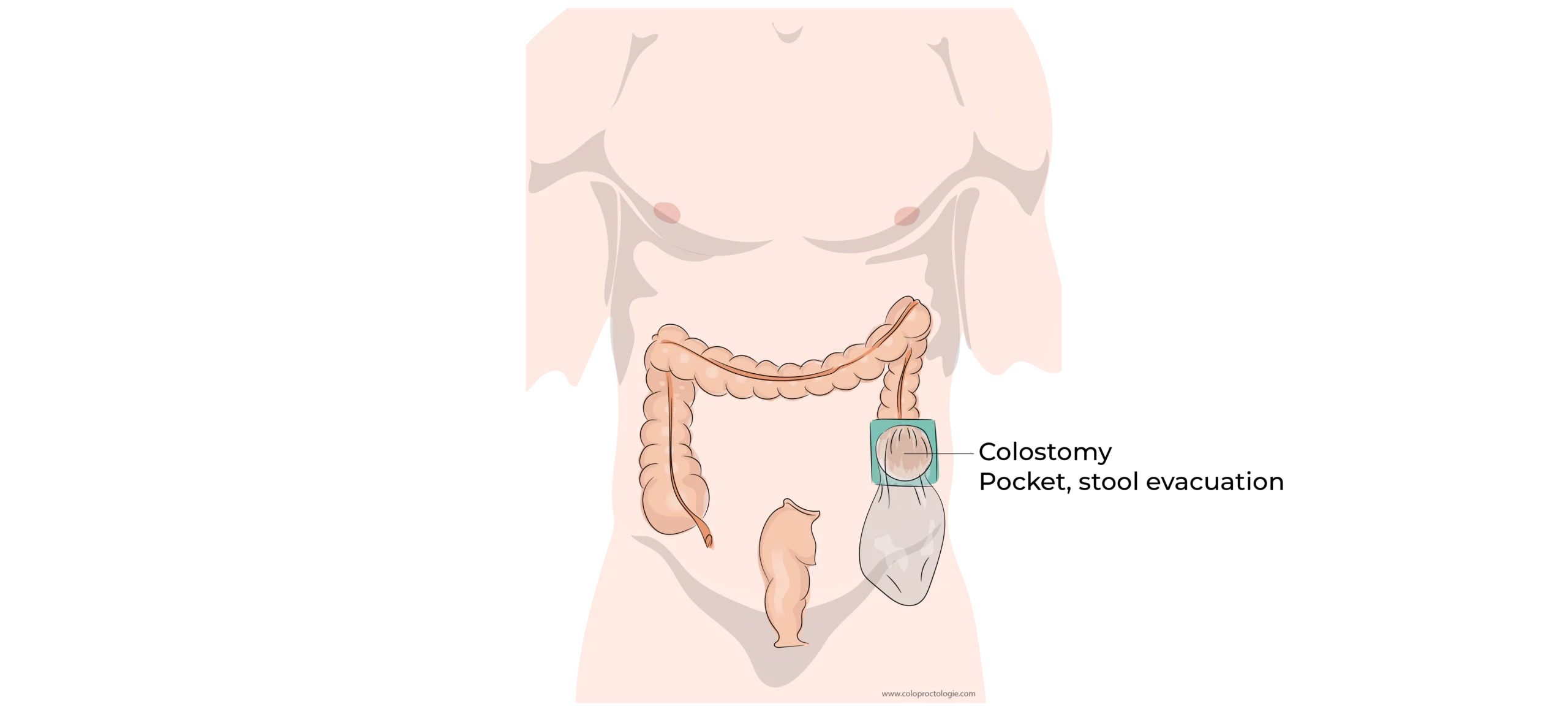
Incidence : < 9 % after laparotomy for abdominal surgery
Adhesions of the small intestine are the main causes of postoperative obstruction. If the obstruction does not clear up spontaneously, surgery may be necessary. Laparoscopic surgery requires less traumatic manipulation of the bowel and causes fewer adhesions. The risk of obstructions is much lower after laparoscopy (keyhole surgery) than after laparotomy (open abdominal surgery).
Incidence : 1,1 – 2,3 %
Incidence : 18 %
Wound infection is common after colon surgery because the colon contains millions/billions of bacteria that may infect the wound. The risk is higher in open surgery than in laparoscopic surgery.
Among other factors, obesity, malnutrition, diabetes and corticosteroids increase the risk of an infection.
Laparoscopy : incidence : 7 %*
Open laparotomy : incidence : 22,4 %*
Wound infection, obesity, malnutrition, diabetes and chronic use of corticosteroids are factors that increase the risk of incisional hernia.
Patients at risk are those requiring anticoagulation medication for cardiovascular disease or those with bleeding disorders.
In most cases, the bleeding stops spontaneously. Treatment by endoscopy (colonoscopy) is rarely necessary.
Incidence : 6,8 %*
After abdominal surgery, the bowel may temporarily lose its ability to contract and expel food, this is called an ileus.
The bowel dilates and the patient can no longer feed. An ileus manifested by discomfort due to the dilated abdomen that may or may not be accompanied by vomiting.
Treatment consists of resting the bowel, inserting a nasogastric probe through which the stomach and bowel are decompressed and stopping morphine analgesics,. The bowel spontaneously returns to normal after 1 to 10 days. On average, postoperative ileus prolongs hospitalization by 4 days. Ileus is more common after laparotomy than after laparoscopy.
The sigmoid (part of the left colon) lies in front of the left ureter. The ureter is the tube that carries urine from the kidney to the bladder. The risk of an accidental injury to the ureter during surgery is rare.
Sometimes resection of part of the ureter (removal) may be necessary in case of invasion of the ureter by tumor.
Incidence : 0,96 %*
During mobilization of the left colon, as a result of traction on the attachments connecting the colon and spleen, tears may occur in the capsule of the spleen. This can lead to bleeding, sometimes requiring removal of the spleen.
Incidence : 3,2 %*
The scar tissue of the he suture between the colon and rectum (distal part of the colon) can contract and narrow the passage. This is called a stenosis.
Usually, a stenosis is treated by one or more endoscopic balloon dilatations. Rarely, another surgical procedure is necessary. A stenosis of the anastomosis seems to be more frequent in men.
In normal conditions, pain is well controlled with paracetamol (Dafalgan®), NSAIDs (anti-inflammatories) or morphine (Tradonal®…) and pain symptoms diminish over time.
If certain symptoms seem abnormal to you contact your doctor.
If this is not possible, you can contact your surgeon.
If you are unable to contact your GP or your surgeon, go to the emergency department at St Elizabeth Hospital in Uccle.
Upon resection (removal) of the left colon, the length of the colon is reduced.
This reduces the postoperative ability to reabsorb water from the stools, so bowel movements may be softer and even liquid immediately after surgery (diarrhea). The remaining colon has enough length to adapt and absorb more water, in subsequent weeks and months the stools can return to a normal consistency.
During surgery, the upper part of the rectum is removed. The rectum acts as a reservoir for stools and ensures a controlled defecation.
After partial removal of the rectum, the ability to hold up large amounts of stool decreases and the patient may experience the need to go to the toilet more frequently with smaller amounts of stool and a softer consistency of stool.
The nerves of the rectum are altered. This may manifest as a feeling of a need to defecate even though the rectum is empty. The patient goes to the toilet although he has no stools in the rectum.
Partial resection of the rectum reduces the patient’s ability to hold stools and episodes of incontinence may sometimes occur.
Conclusion
Immediately after surgery, the patient will have softer and more frequent stools with a risk of incontinence episodes. In the weeks and months after surgery, frequency becomes more regular and stools usually normalize.
While dissecting the artery feeding the sigmoid and left colon, the nerve plexus (network of nerve fibers) or a nerve (superior hypogastric) may be injured resulting in sexual dysfunction.
If both nerves or if the plexus is completely severed, it leads to anejaculation (= the man’s inability to secrete sperm despite normal erection and stimulation). This nerve injury does not prevent erections, sexual relations and orgasms.
In women, vaginal dryness and pain during intercourse may be present after injury to the nerves.


